Innovating Patient Care
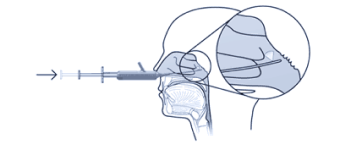
Tx360EU Nasal Applicator

E.U. Patent No.
EP 2640450B1/ EP 232637B1
Precise targeting, for optimal results
Patented technology targets the SPG nerves to alter its signals
Delivering medication precisely and consistently to the SPG, with ease, every time
Minimal medication,
Maximum effect
Watch How the Tx360EU Works
About Tian Medical

Your Health, Our Mission:
Trusted Physicians, Transformative Care
Your Health, Our Mission:
Trusted Physicians, Transformative Care
I am a medical professional
Professional Partnerships Welcome
I am a medical professional
Professional Partnerships Welcome
I am an individual
Learn more about the Tx360®
Thank you for your interest in Tx360
To nominate your provider to be trained on Tx360
Hear from Our Community:
Real Success Stories with Tx360EU
We found the procedure to be very easy to learn and quick to administer while providing good outcomes.
Given the overwhelming success of this treatment, we plan to continue using the Tx360 in our clinics and in the Urgent Care.
The procedure has allowed me to stay away from using over-the-counter medications and prescriptions, longer than anything else I’ve tried.
SPG procedures have given me the biggest window of relief, which has reduced the amount of time I’ve had to take off work.
The application of the nasal catheter isn’t painful at all. I would have these treatments again.
We found the procedure to be very easy to learn and quick to administer while providing good outcomes.
Given the overwhelming success of this treatment, we plan to continue using the Tx360 in our clinics and in the Urgent Care.
The procedure has allowed me to stay away from using over-the-counter medications and prescriptions, longer than anything else I’ve tried.
SPG procedures have given me the biggest window of relief, which has reduced the amount of time I’ve had to take off work.
The application of the nasal catheter isn’t painful at all. I would have these treatments again.